Leg edema directly affects circulation, mobility, and cardiovascular health. Prolonged swelling is often accompanied by a feeling of heaviness in the legs, skin tightness, and increasing fatigue.
Cardiologists from the American Heart Association emphasize that leg edema can reflect several important disorders involving the heart, kidneys, and venous system. Many recent studies have also noted that prolonged fluid retention increases the risk of soft-tissue damage, dermatitis, and impaired lower-extremity circulation.
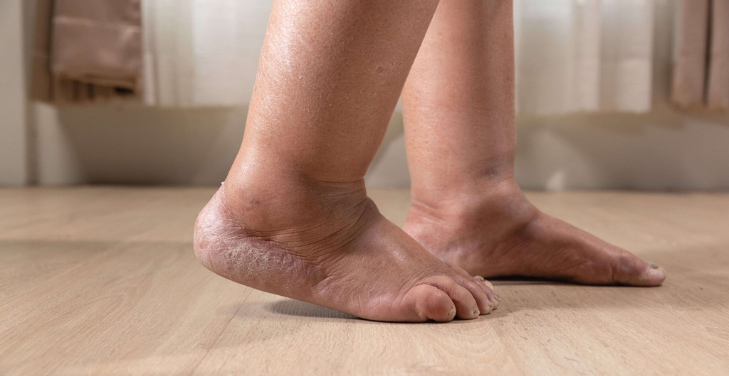
Persistent leg swelling may signal circulation problems, infection, or dangerous underlying health conditions.
What Is Edema in the Legs?
Leg edema occurs when fluid accumulates in the tissues of the feet, ankles, or lower legs, creating a feeling of heaviness, tightness, and noticeable swelling. This condition often develops silently but significantly affects circulation, mobility, and cardiovascular health.
Fluid Accumulation in Leg Tissues
The circulatory system constantly transports fluid between blood vessels and soft tissues. When venous pressure increases or the lymphatic system becomes inefficient, fluid quickly accumulates under the skin. The legs are most affected by gravity, which pulls fluid down the lower part of the body throughout the day.
Common Physical Signs
Patients often feel their skin is taut and shiny, their legs feel heavy, and their shoes feel tighter than usual. In some cases, an indentation appears after pressing on the skin for a few seconds. Swelling increases towards the end of the day, especially after prolonged standing or sitting.
Why Leg Edema Matters
Leg edema reflects many important disorders related to the heart, kidneys, liver, or venous circulation. Prolonged edema reduces blood flow, increases tissue pressure, and promotes chronic skin damage.
Common Causes of Leg Edema
Leg edema stems from various internal mechanisms. Changes in circulatory pressure, organ dysfunction, and daily lifestyle habits all contribute to fluid accumulation in the lower extremities. The degree of swelling usually increases over time and significantly affects mobility.
Venous Circulation Problems
The venous system returns blood from the legs to the heart. When venous valves weaken, blood pools in the lower legs, significantly increasing pressure within the vessels. Fluid quickly escapes from the blood vessels into the soft tissues, creating a feeling of heaviness and prolonged tightness in the legs.
Heart and Kidney Conditions
The heart and kidneys control blood flow and fluid balance in the body. Heart failure slows circulation, while impaired kidney function leads to continuous accumulation of sodium and water. Leg edema is often more noticeable in the evening, accompanied by fatigue and tightness around the ankles.
Lifestyle and Medication Factors
Prolonged sitting or standing and a high-salt diet cause the body to retain more water. Certain blood pressure medications, corticosteroids, or hormones also promote swelling in the legs by altering blood pressure and retaining fluid in tissues.
Early Symptoms That Should Not Be Ignored
Early signs of leg swelling are often mild but progress rapidly over time. The body sends warning signals through changes in the skin, a feeling of heaviness in the legs, and reduced daily mobility. Early recognition allows for more effective control of the underlying cause.
Swelling Around the Ankles
The ankle area is often noticeably swollen at the end of the day, especially after many hours of continuous standing or sitting. Shoes become tighter, the skin feels taut, and a heavy, constricting feeling develops around the ankle. Some people notice sock marks lasting longer than usual.
Skin Texture Changes
The skin on the legs becomes shinier, tighter, and more sensitive to touch. Fluid accumulates in the tissue, creating an indentation after a few seconds of light finger pressure. This change reflects the increasing fluid pressure beneath the skin's surface.
Heaviness and Leg Fatigue
Patients often feel their legs tire quickly, walk with a heavy gait, and experience reduced endurance during activity. A feeling of tightness radiating down the calf makes everyday activities more difficult in the afternoon or evening.
Dangers of Untreated Edema in Legs
Prolonged leg swelling creates constant pressure on blood vessels, soft tissues, and skin surfaces. Chronic swelling progressively impairs circulation, promoting a range of serious complications related to infection, tissue damage, and reduced mobility.
Chronic Skin Damage
Excess fluid causes the skin to become taut, thin, and more vulnerable over time. Areas around the ankles often appear dry, discolored, or cracked. Small wounds quickly develop into ulcers due to continuously increased tissue pressure and reduced blood flow.
Increased Risk of Infection
Fluid buildup creates a favorable environment for bacteria to thrive in soft tissues. Swollen areas of the legs become hot, red, and painful, and inflammation can spread when skin infections occur. Some cases progress to cellulitis very rapidly.
Reduced Mobility and Circulation
Prolonged leg heaviness reduces walking endurance and limits daily activity. Slower blood flow in the veins continues to exert pressure on the lower extremities, leading to increasingly severe leg swelling.
When Leg Swelling Signals a Medical Emergency
Some cases of leg swelling develop extremely rapidly and reflect a dangerous internal medical emergency. Accompanying signs are often directly related to blood clots, acute heart failure, or widespread infection. Early recognition significantly reduces the risk of life-threatening complications.
Sudden Swelling in One Leg
Sudden swelling in one leg is often associated with deep vein thrombosis. The affected leg becomes stiff, painful, and noticeably warm to the touch. The blood clot obstructs blood flow and poses a high risk of pulmonary embolism.
Chest Pain and Breathing Difficulty
Leg swelling accompanied by chest pain or difficulty breathing indicates severe stress on the cardiovascular system. Reduced heart pumping capacity causes fluid to accumulate rapidly in the legs and lungs. Patients often experience shortness of breath, rapid heartbeat, and extreme fatigue after even light activity.
Rapid Skin Color Changes
Leg skin turning dark red, purple, or pale reflects an acute circulatory disorder. These color changes often accompany a burning sensation, intense pain, and widespread tightness around the swollen area.
Conditions Commonly Linked to Severe Leg Edema
Severe leg edema often reflects underlying disorders of the cardiovascular, renal, or lymphatic systems. The persistent swelling is accompanied by a feeling of tightness and heaviness in the legs, as well as noticeable skin changes. Many chronic conditions lead to persistent fluid accumulation in the lower extremities and, over time, impair circulation.
Congestive Heart Failure
Congestive heart failure reduces the heart's ability to pump blood throughout the body. Blood pools in the veins, causing a significant increase in pressure in the legs and ankles. Fluid quickly escapes from the soft tissues, resulting in more noticeable swelling at the end of the day or after exercise.
Kidney Disease and Fluid Retention
The kidneys control the body's salt and water levels through continuous blood filtration. When kidney function declines, excess sodium and fluid accumulate heavily in the subcutaneous tissue. Patients often experience leg edema, fatigue, rapid weight gain, and taut, shiny skin.
Lymphedema and Lymphatic Dysfunction
The lymphatic system carries excess fluid away from soft tissues. Disorders of lymphatic flow cause persistent accumulation of protein-rich fluid in the legs, resulting in a feeling of heaviness, stiffness, and swelling that can last for months.
How Doctors Diagnose the Cause of Leg Edema
Diagnosing leg edema requires a comprehensive assessment to accurately determine the cause of fluid accumulation. Doctors typically combine clinical examination, laboratory tests, and imaging to assess circulation, organ function, and the extent of soft tissue damage. Every small sign is important in guiding the diagnosis of the underlying condition.
Physical Examination Findings
Doctors examine the degree of swelling, skin color, and the leg area's temperature to assess circulation. Indentation after pressing on the skin helps determine the amount of fluid accumulated in the tissue. Heart rate, blood pressure, and the presence of prominent veins also provide important data on cardiovascular health and blood circulation.
Blood and Urine Testing
Blood tests help assess kidney and liver function, as well as protein levels in the body. Some indicators directly reflect the presence of heart failure or ongoing inflammation. Urine analysis helps detect protein loss or fluid retention disorders.
Imaging and Ultrasound Scans
Doppler ultrasound allows visualization of blood flow in leg veins and rapid detection of blood clots. X-rays or echocardiograms help assess heart function, lung conditions, and fluid retention.
Treatment Options for Leg Edema
Treatment for leg edema focuses on reducing fluid buildup, improving circulation, and controlling the underlying cause. The right regimen helps reduce leg heaviness, supports mobility, and limits long-term tissue damage. Treatment effectiveness is often significantly enhanced when combined with lifestyle changes and specialized medical care.
Compression and Leg Elevation
Compression stockings help veins return blood to the heart more effectively, thereby reducing swelling and leg tightness. Elevating the legs while resting improves fluid circulation and reduces pressure on the ankles. Many people feel lighter in their legs after just a few days of consistent use.
Medications and Fluid Control
Diuretics help the body eliminate excess water and sodium through the urinary system. Doctors usually adjust medication based on an individual's heart, kidney, and blood pressure conditions. A low-salt diet also helps control fluid buildup in soft tissues.
Treating the Underlying Disease
Controlling heart failure, kidney disease, or venous disorders has a long-term impact on chronic leg edema. Treating the underlying cause improves circulation and reduces the risk of future edema recurrence.
Ways to Reduce the Risk of Future Swelling
Long-term control of leg swelling depends heavily on daily habits and the ability to maintain stable circulation. Small changes in exercise, nutrition, and body care have a strong impact on fluid circulation and venous health.
Stay Physically Active
Regular physical activity promotes stronger leg muscle contractions, thereby helping blood return to the heart more effectively. Walking, cycling, or swimming helps reduce pressure in the veins and improve fluid circulation in the lower extremities. The feeling of heavy legs also significantly decreases after maintaining regular activity.
Manage Sodium and Body Weight
High salt intake causes the body to retain more water, increasing the likelihood of swelling. A balanced diet and stable weight help reduce pressure on blood vessels and the lymphatic system. The heart and kidneys also function more efficiently when the body maintains a healthy metabolic state.
Improve Daily Leg Circulation
Elevating your legs while resting helps improve blood flow in the lower legs and ankles. Changing positions frequently throughout the day helps reduce circulatory stagnation and prevent prolonged fluid buildup.
Conclusion
Leg swelling reflects several significant changes in circulation, cardiovascular health, and fluid balance. Prolonged swelling severely impairs mobility, soft-tissue health, and daily quality of life.
Early recognition of warning signs leads to more effective treatment. Regular exercise, a balanced diet, and proper circulatory care help reduce the risk of future leg swelling recurrence.
Regular monitoring helps detect abnormalities quickly and protects long-term health.
Frequently Asked Questions (FAQs)
- Can leg edema become dangerous? – Prolonged leg edema increases pressure on veins, skin, and soft tissues, contributing to inflammation, ulcers, circulation problems, and conditions linked to heart failure or deep vein thrombosis.
- Why does leg swelling worsen at night? – Gravity causes fluid to collect in the lower legs throughout the day, increasing venous pressure and making swelling, heaviness, and tightness more noticeable in the evening.
- Which foods help reduce fluid retention? – Potassium-rich foods such as bananas, avocados, and leafy greens support fluid balance, while lower sodium intake and proper hydration help reduce water retention.
- Does walking improve leg edema? – Walking activates leg muscles and improves blood return to the heart, helping reduce venous pressure, fluid buildup, and feelings of leg heaviness.
- When should someone seek medical attention? – Sudden swelling, severe pain, shortness of breath, chest pain, or rapid skin discoloration may signal serious circulatory complications and require prompt medical evaluation.

